When End-Stage or Recurrent Gynecologic Disease Leaves Few Options, PRISM Extends What’s Possible.
When guideline-based care reaches its limits, PRISM helps reveal the deeper systems driving disease progression — giving clinicians a new path to stabilizing complex cases.
From Guidelines to Systems Thinking: Why PRISM Changes the Clinical Outcome
Standard Gynecologic Care Is Essential — But It Reaches a Limit in Advanced Disease
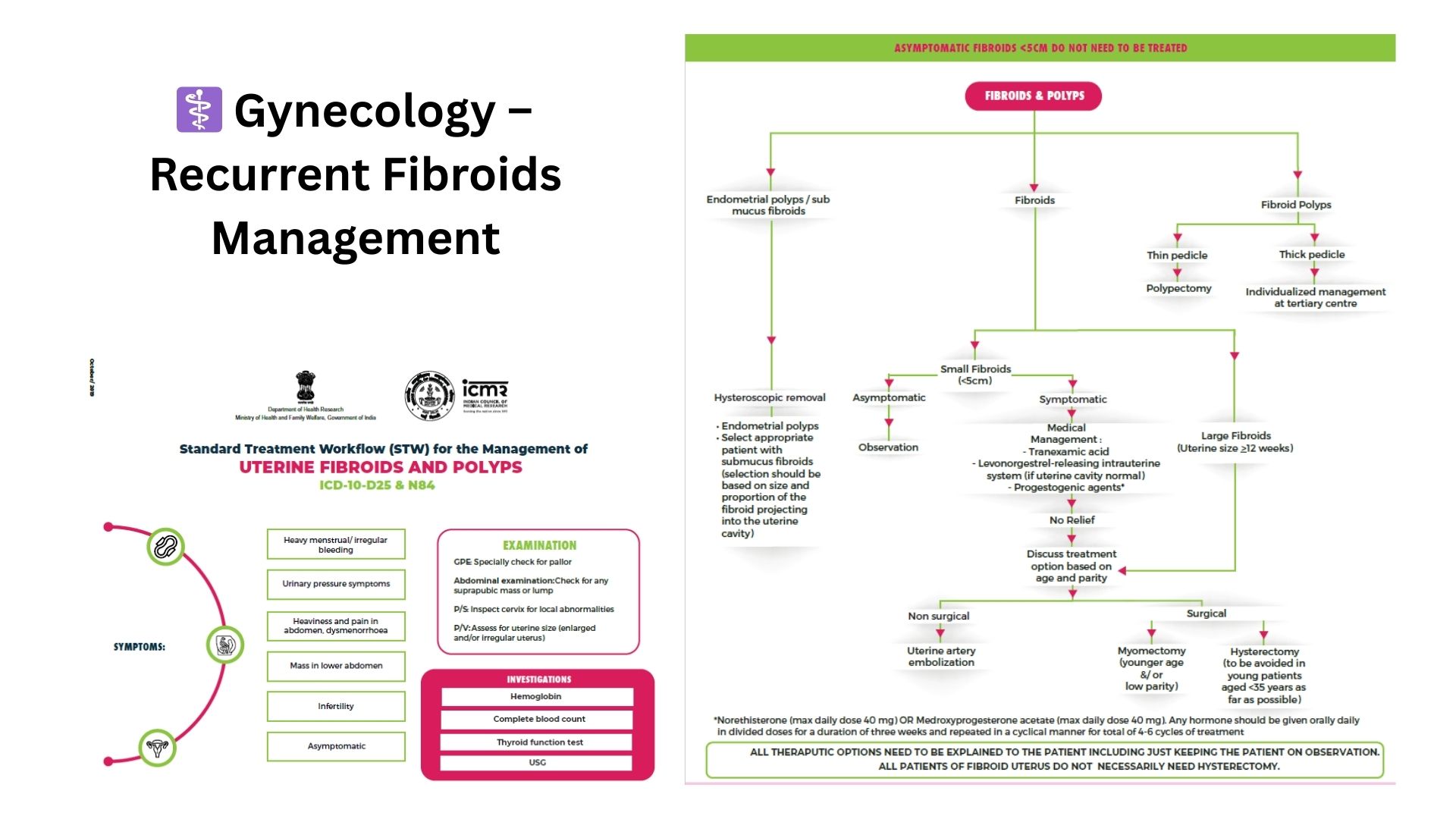
Guideline-directed gynecologic management prioritizes curative pathways: staged surgeries, chemoradiation protocols, hormonal suppression for endometriosis, and structured evaluation of pelvic pain syndromes.
These approaches work for early and intermediate disease, but once a patient reaches recurrent ovarian/cervical cancer post-therapy exhaustion, refractory endometriosis with organ involvement, or severe pelvic pain syndromes causing functional collapse — the guideline algorithm provides fewer options.
Progression in these patients is often driven by deeper systemic dysfunctions that linear gynecologic pathways cannot address:
- Immune–inflammatory loops sustaining tumor or pain activity
- Neuro-hormonal imbalance influencing pelvic pain and fatigue
- Gut–pelvic microbiome cross-talk affecting inflammation and recurrence
- Metabolic and mitochondrial stress driving cachexia and exhaustion
- Autonomic dysregulation amplifying pain perception
- Phenotype-specific vulnerability shaping disease progression
These system-level contributors are never evaluated in standard gynecologic guidelines.
Where Traditional Approaches Fall Short
Recurrent gynecologic cancers post-curative exhaustion
When surgery, radiotherapy, and chemotherapy have all been maximized, patients continue to decline due to systemic inflammatory and metabolic drivers that guidelines do not address.
Refractory endometriosis with organ involvement
Pain, bowel/bladder dysfunction, and systemic inflammation persist even after hormonal suppression or multiple surgeries because the root immune–metabolic loops remain untreated.
Chronic pelvic pain syndromes with functional collapse
Neuro-visceral sensitization, autonomic imbalance, microbiome effects, and phenotype patterns amplify symptoms long after guideline-level therapies are exhausted.
PRISM: A Systems Medicine Lens for Complex Gynecologic Disease
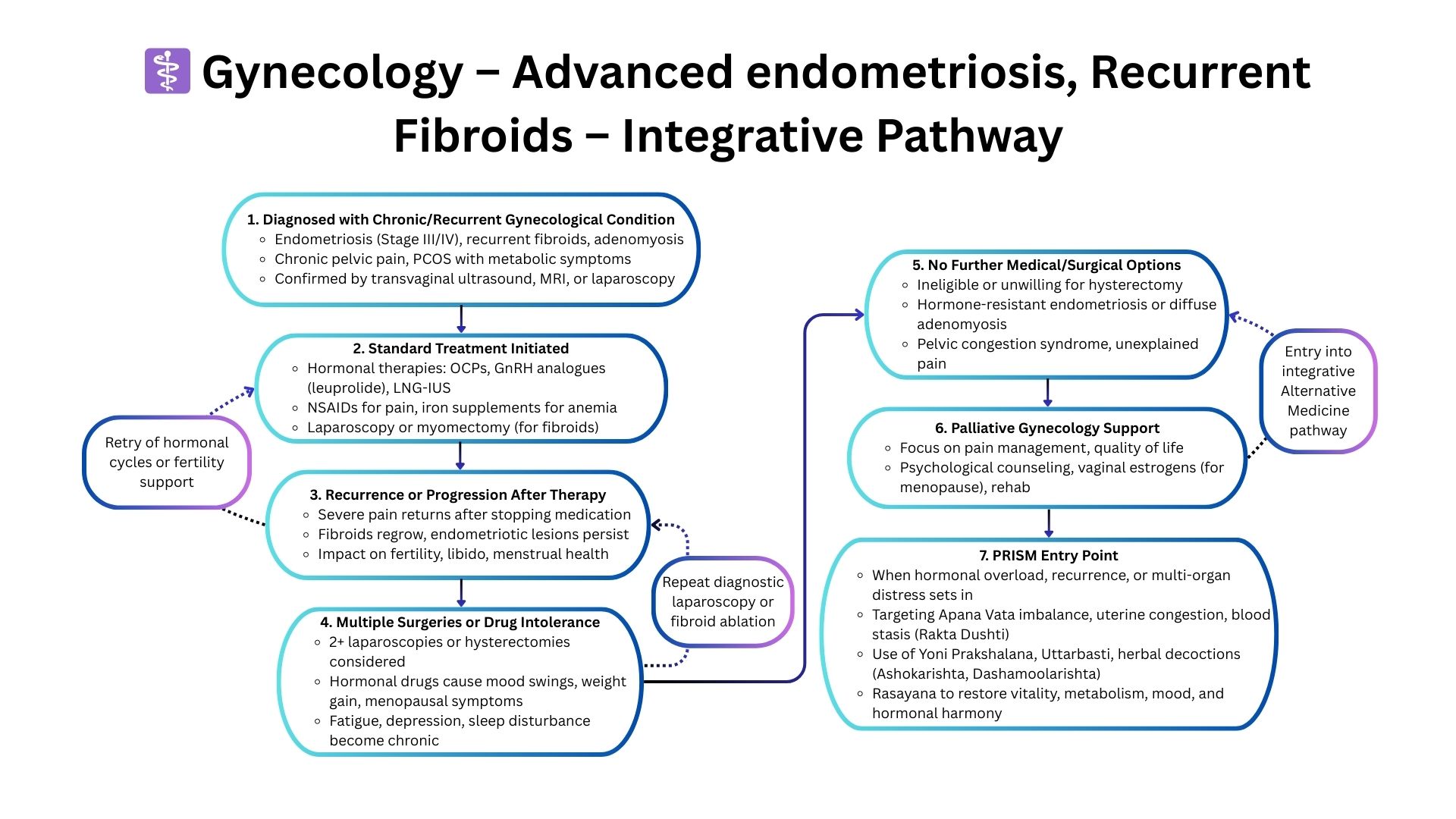
Why PRISM Works When Gynecology Guidelines Stop
PRISM goes beyond tumor-directed or organ-focused treatment, revealing the systems-level forces that sustain progression:
- Immune–inflammatory circuits fueling tumor activity or endometriosis
- Neuro-autonomic dysregulation amplifying chronic pelvic pain
- Gut–pelvic microbiome interaction affecting recurrence and inflammation
- Mitochondrial and metabolic stress worsening fatigue and cachexia
- Hormone–immune–neural linkage driving symptom oscillations
- Phenotype-based stratification guiding personalized intervention priorities
With this systems map, clinicians can stabilize decline, reduce pain, improve energy, and identify actionable biological drivers — even when traditional gynecologic oncology or endometriosis pathways offer no further options.
